How Mobile Phones Cause Neck, Back Pain & Headaches
Health providers across the globe have become quite familiar with the body’s response to the new technology of the 21st Century, and the last two years appear to have had a considerable impact on our joints and alignment in the hands, neck, shoulders, and upper backs including additional loading on the low back.
In conversations with our patients, we have noted a great deal of poor ergonomic desk setup that has occurred due to working at home requirements during the lockdowns, as well as greater demands of the companies/businesses on their employees, equating to more time in front of a computer, often with poor posture adaption.
Most students have spent more time in their rooms, particularly in the last two years. Laptop usage at school has also become commonplace. These days, most teenagers and University students lives revolve around staring at their laptops or their phones. This is not new information for everyone!
The Rise of Technology and Strain on the Body
The rise of technology accessibility and overuse, plus the consequence of lockdowns, have caused a great increase in complaints such as back pain, neck pain, headaches, shoulder pain and repetitive type strain injuries.
Tendinitis in the fingers, thumbs, wrists, elbows and all the way up the arm to the neck can result from tapping away on mobile phones. We are using our muscles and joints in ways that strain them. Wrists are flexed for long periods, holding too much weight, with fingers moving repeatedly across a very short range of motion. The head is often flexed forward changing the load onto joints and muscles. Over time, these actions can cause inflammation and pain. For example, studies have been done linking De Quervains tenosynovitis (tenosynovitis of the thumb) to mobile phone usage. The pinkie finger is often used to hold the weight of the phone also leading to problems.
Text Neck
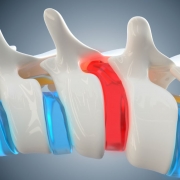
From a clinical perspective, the greatest issue with mobile phone usage is headaches, neck pain and upper back pain, as the fulcrum of the head and neck tends to load up the joints and muscles in the upper back and lower neck causing strain here, as well as under the base of the skull from the muscle pull. Text neck or forward head carriage can load the neck muscles and cervical spine by a factor of 4 to 5! 10cm of forward head carriage (the ear forward of the tip of the shoulder) adds 4.5 kilograms on to the top of the shoulders. Ouch! Be aware of that word document or zoom call where you are leaning into your screen.
Very frequent phone usage can also affect the nerve at the elbow, the ulnar nerve. The symptomatic picture of this is numbness and weakness in the pinkie finger and ring fingers. However, loading the discs and nerves in the lower neck and upper back can also induce these symptoms. Anytime there is inflammation, there is also swelling. This can cause a squeeze on the nerves that run through them. Imagine standing on a hose.
Wear Tear and Pain
It is always important to remember that postural alterations could also exacerbate pre-existing nerve and joint issues. Our body, in a correct postural stance, free of any injury that has not caused a change in any of our normal curves of our spine, has a center of gravity that enables even weight distribution on the joints and a relative relaxation of muscle tissue and ligaments. A simple analogy is a wheel alignment in a car. If you hit a curve badly, or are involved in a collision, the wheels and often the body of the car can be very altered. The tyres start to wear. The same applies to the spine. Imagine the implications of a building foundation that was not stable. Once areas of the spine or joints in the body take a greater load, then wear and tear will develop.
Sleep Issues
Blue light from our screens can also disrupt our circadian rhythms and therefore our sleep. Blue light affects the production of melatonin in our bodies reducing both the quality and quantity of sleep. Blue light glasses can help to block some of this light. Many companies will have different shapes and sizes to choose from as well as provide magnification if that is also required for reading.
Solutions
We’ve seen an ever increasing frequency of such issues at our Lane Cove chiro clinic. The good news is that much can be done to improve these issues with new technology. It is never too late to implement some change. Most of the lack of good joint movement and therefore the development of pain we see in practice is from poor loading patterns. The muscles are like cables and will adapt to what the structure is doing (think the Leaning Tower of Pisa). Simple chiropractic adjustments and adoption of healthy postural control can remedy many symptoms. There are also numerous devices on the market than can help restore normal spinal curves. Postural muscle strengthening is also key. Accelerated disc degeneration can result in any changes, so if you catch things early, they don’t tend to become chronic.
What You Can Do:
- Microbreaks – Take regular breaks to unload. Recommended 30 seconds every hour. Neck retraction, arms by your side, turning your thumbs out and holding your shoulders back for a 30 second hold can prevent repetitive strain on joints, ligaments and muscles. Also find time in the day where you think about how you are holding your body and fix it. Hopefully, with enough practice, it will become subconscious.
- Invest in a large foam roller – Lie on it vertically, head resting, knees bent, feet flat on the floor, dropping the arms back, opening the chest. This is also brilliant to calm the nervous system and can be helpful before bed to rest the mind.
- Learn to strengthen your shoulder blade stabilisers – Ideally starting with a theraband. It is important to keep these muscles switched on when working on a computer. This can prevent many shoulder injuries, including rotator cuff.
- Mobilise – Broomstick rotations, wall angels, knee to chest pull ups, hip rolls, neck rotations.
- Improve the home office setup – Standing workstations relieve the pressure on the low back tremendously. It is very important to have your eyes looking straight ahead so improving screen height is essential and this includes laptops. Improve the keyboard so your elbows remain at 90degrees and are not extended out (this causes rounding of the shoulders) and adopt the use of a better mouse or wrist support.
- Voice to text option for mobile phones and hold the phone up! – Use phone grips.
- Tone Up with Pilates or Gym or do some Yoga – Without the concrete pillars in a building, what’s going to hold it up?
- Regular Chiropractic adjustments – Free joint movement, balancing the body’s biomechanics, unloading discs and nerves will also relax the muscles, keeping yourself tuned. Here, unlike dental work or your car mechanic, we can’t replace the parts, so get tuned up!